This is an archived article that was published on sltrib.com in 2013, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
Laura Privett is worried about the future of her children's very expensive mouths.
Her eldest, 16-year-old Wade, got his first filling before he turned 4. Her youngest, 6-year-old Kayden, was born with a partial cleft lip and had his first dental x-rays at five days old. He's already had cranial facial surgery, six fillings and six caps. His jaw is so overcrowded with aching teeth that sometimes he can't eat.
"If it wasn't for Medicaid, my kids would not have access to those dental services," the Kearns mother said.
The care the Privetts rely on may change under a state plan to hire private managed care organizations to run the Medicaid dental program. Utah pediatric dentists fear the move will mean less access to care for children and smaller payments for dentists.
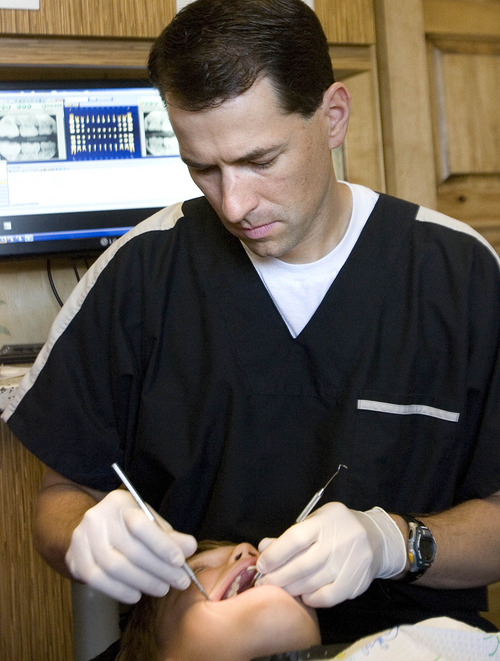
Privett's pediatric dentist, Jason Horgesheimer, is leading the opposition.
"We feel like privatizing introduces an entirely new challenge and hurdles for the children to receive their dental care," said Horgesheimer, president of the Utah Academy of Pediatric Dentistry, which represents 85 pediatric dentists statewide.
The change, which affects dentists in Davis, Salt Lake, Utah and Weber counties, has been approved by the Centers for Medicaid and Medicare and is set to take place on Sept. 1. State health officials project savings of $2 million — an estimate that doesn't factor in an expected increase in Medicaid enrollment when rules of the Affordable Care Act (ACA) kick in come January.
"Managed care can help give more fixed costs for the state so we know how to budget," said Rep. Jim Dunnigan, R-Taylorsville, whose 2011 legislation prompted the switch. "We need to have a greater emphasis on preventative care and less on restorative care, which is very expensive."
Horgesheimer said dentists worry they will lose money under the new system and will have to drop out of Medicaid, leaving kids without care. He predicts care will be delayed because more procedures will require pre-approval and some patients may have to seek new providers.
State officials, who contend neither dentists nor children will be shortchanged, met Tuesday with dentists and the two companies with the new contracts — Delta Dental and Premier Access. After the meeting, Dunnigan said he believes the transition will not be as disruptive as dentists fear.
The plans offer dentists two payment options:
• In the capitated system, dentists will receive a monthly flat fee of $5 or about $10 per patient, whether the patients are treated or not.
• Under the fee-for-service plan, dentists will be paid each time a child is treated, at rates set by the plans.
Like Medicaid, which covers 40 percent of what dentists regularly charge patients, the plan rates would cover less than the dentists' usual prices and less than rates paid by private insurance. Representatives of both plans said their proposed rates are the same as those paid by Medicaid.
All of Utah's Medicaid medical care, and both medical and dental care from the Children's Health Insurance Program (CHIP), which covers low-income kids, are provided through managed care. The dental program is "an outlier," so the change makes sense, Duningan said.
The CHIP transition to managed care was bumpy but has worked well and saved the state money, he said.
But Horgesheimer questions whether managed care can work in dentistry, where much of the care is driven by procedure work.
Many of the children seen by pediatric dentists, who have more specialized skills than general dentists, have teeth so rotted with decay and disease that their general health is threatened, he said.
Horgesheimer, whose dental practice has as many as 3,000 Medicaid patients, contends most dentists have said they renewed their Medicaid contracts without understanding the changes. He claims that as dentists get more information, they are dropping out of the program.
Sen. Allen Christensen, R-North Ogden, a retired pediatric dentist, said Tuesday at a Social Services Appropriations subcommittee meeting in Garland that he is skeptical about the access kids will have to pediatric dentists. With the low pay under the capitated system, the "only way [pediatric dentists] can manage it is by not seeing the patient as much as they ought to," he said.
After the expected boost in Medicaid enrollment under the ACA, "with all the new patients coming on board, it's not going to work," Christensen said.
But state officials believe there should be adequate access because the plans have hired more than 400 dentists, including at least 17 pediatric dentists, said Emma Chacon, the health department's director of the Bureau of Managed Health Care.
Medicaid enrollees can continue to see their dentists — if their provider has signed up with the plans — or will be assigned a dentist near their residence, Chacon said. They'll also be allowed to switch providers if they are unhappy, she said.
Advocates for the poor say they will sound the alarm with state leaders if access becomes an issue.
"We expect that the Department of Health will make sure the contracted plan preserves a high level of access to dentists," said Matt Slonaker of the Utah Health Policy Project. "Many of these children have great dental health needs and not being able to see their dentist would be extremely disruptive."
That's just what Privett fears. Through braces and tooth extractions and even more fillings, her kids have reacted poorly to changes in their care providers. If she loses access to her dentist — or to coverage in general — she's not sure what the family will do, even though they have some limited coverage through her husband's job.
"I don't think (managed care) is a good idea," she said. "My six-year-old has so much major dental work ahead of him. If the dentists aren't getting paid enough compensation in order for them to treat my son and I can't afford to treat him, he's going to lose all his teeth."
Tribune reporter Kristen Moulton contributed to this report. —
The dental safety net
Utah paid just over $37 million in Medicaid dental claims in 2012, covering more than 2.1 million dental visits for the roughly 134,000 pregnant women and children who qualify. Pediatric care makes up the majority of the claims.