This is an archived article that was published on sltrib.com in 2017, and information in the article may be outdated. It is provided only for personal research purposes and may not be reprinted.
When doctors confirmed Tommy Tanzer's prostate cancer diagnosis, relief washed over him.
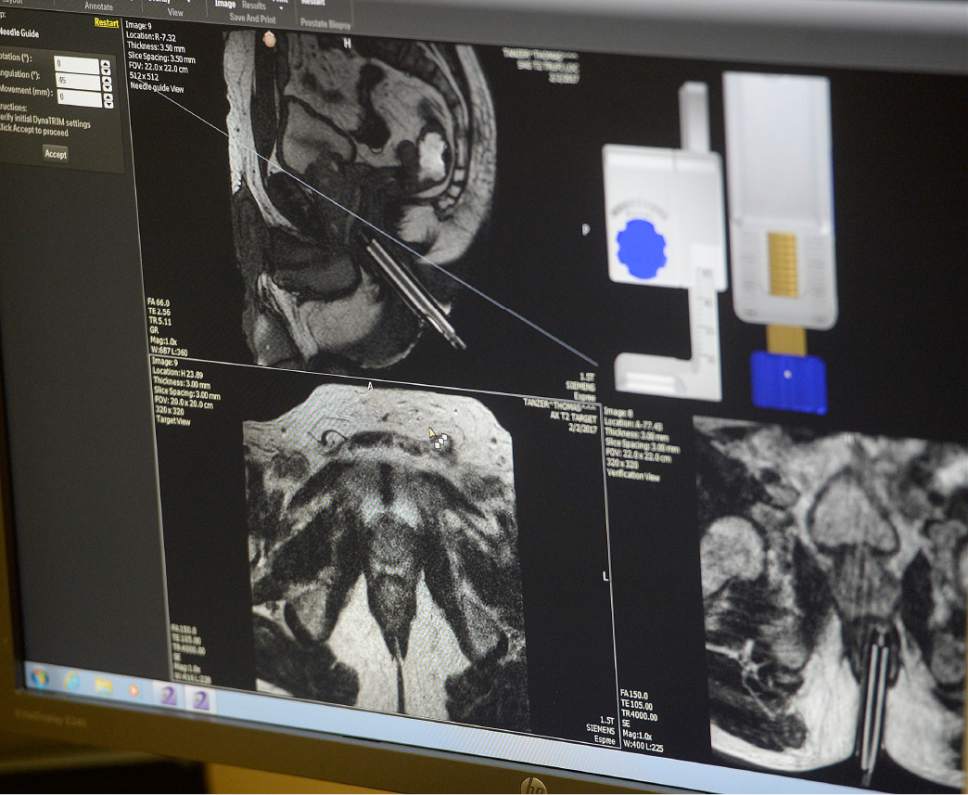
Previous biopsies repeatedly came back negative for cancer, even though the 67-year-old's blood tests continued to indicate he might have the disease. But a new test in early February relied on a precise imaging device used in tandem with the biopsy, letting doctors at the Huntsman Cancer Institute pinpoint their tissue samples more accurately.
"I got a call from my doctor saying, 'We have good news and bad news,' " Tanzer, a Park City resident, recalled. " 'The good news is you're going to be perfectly fine and treatable. The bad news is we found the cancer.' "
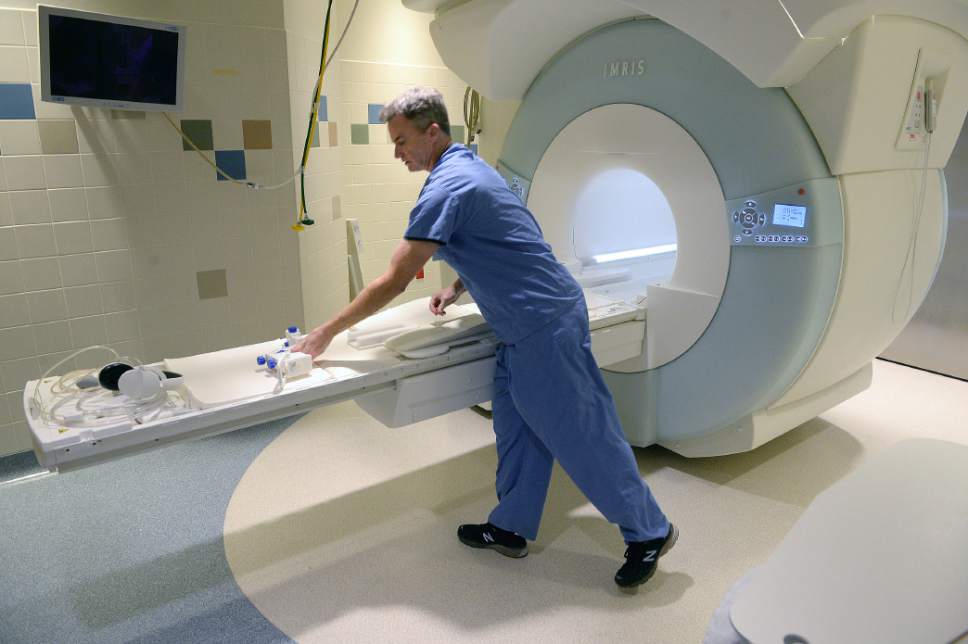
The new technique for MRI-guided prostate biopsies has been in use for about a year at the Salt Lake City-based institute, the only hospital in Utah with the technology.
In more traditional biopsies, a urologist uses an ultrasound to view of the prostate but can't generally see cancer. Twelve to 14 blind biopsies are usually taken from six regions in the prostate in the hope of finding a cancerous lesion.
Tanzer likened his own past biopsies to "using a garlic grater and taking a chance."
But coupling the tests with magnetic resonance imaging gives a more accurate view of abnormalities in the prostate, allowing for only one to three biopsies into those specific regions, said Rulon Hardman, the lone radiologist at the institute to specialize in MRI-guided biopsy.
One in seven men will be diagnosed with prostate cancer in their lifetimes, according to the American Cancer Society.
Patients using the new testing technology receive a preliminary MRI before the biopsy so doctors can spot potential cancer lesions. They then return to the MRI machine under conscious sedation for what is about a 30-minute procedure.
Hardman has performed scores of MRI-guided biopsies since the Huntsman Cancer Institute purchased the equipment, noting that none of his patients has experienced complications thus far.
The procedure, he said, is primarily used on patients like Tanzer, with multiple negative biopsy results despite blood tests indicating that levels of the cancer-indicating prostate-specific antigen, or PSA, continue to rise.
Hardman added the method locates cancer lesions about 85 percent of the time, compared with a 44 percent location rate with traditional biopsies.
With the new technique, "we can see where we couldn't before," Hardman said. "I don't know of any other cancers where you need to blindly stick people with a needle. Imagine if we did this for women with breast cancer."
There are a limited number of hospitals throughout the country that have the MRI-guided biopsy method at their disposal. The closest other facilities to Utah using this method are in San Francisco and Oregon.
Intermountain Healthcare's Urological Institute in Utah uses a similar technique called MRI fusion biopsy, also geared toward patients who have had multiple negative biopsy results. Physicians create a 3-D image of the prostate using an MRI that is then combined with real-time ultrasound images to guide biopsies toward potential cancerous regions.
The method has been in use for about 16 months, said Jay Bishoff, medical director of the Urological Institute. Procedures take about 10 to 15 minutes in his office.
"Now that we have the MRI fusion involved, it's been extremely helpful," Bishoff said. "We are finding more aggressive cancer early enough and can make even more informed decisions on surveillance and treatment."
In Tanzer's case, the MRI-guided biopsy in February not only dispelled uncertainty about his cancer, it also prompted swift radiation treatment. His radiation oncologist at Huntsman Cancer Institute, Jonathan Tward, predicted that Tanzer has a 95 percent chance his cancer won't return as doctors monitor him over the next decade.
The MRI-guided biopsy, Tward said, "ended a multiyear frustrating tale for Tommy. I could finally direct appropriate treatment for him."
Twitter: @kelgiffo